Bad breath, or halitosis, impacts social confidence and health, with 80-90% of cases originating in the mouth from bacteria producing volatile sulfur compounds (VSCs) by breaking down food particles, saliva, and cells.
This comprehensive guide outlines six key causes based on dental and medical insights, providing practical, evidence-informed solutions to restore fresh breath. Regular oral care and professional check-ups form the foundation for prevention.
1) Poor Oral Hygiene and Plaque Buildup
The leading cause of bad breath is inadequate cleaning, allowing plaque (bacterial film) and food debris to accumulate, fostering VSC-producing bacteria. This affects teeth, gums, and hard-to-reach areas like the back molars.
Solution: Brush twice daily for 2-3 minutes using the 3-3-3 rule—after meals, within 3 minutes, for 3 minutes—covering all surfaces, including inner molars with interdental brushes. Floss daily and use interdental brushes for gaps. Schedule professional scaling every 6 months to remove tartar.
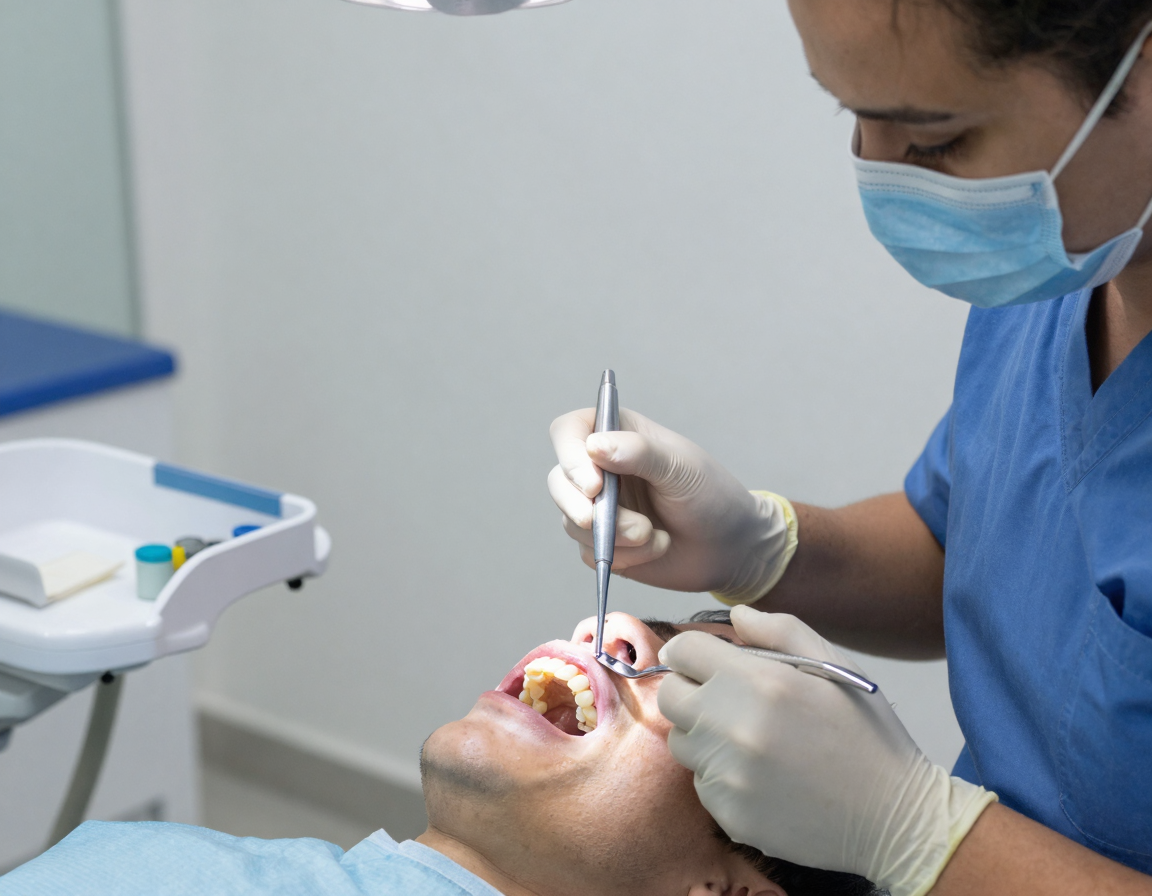
2) Dental Issues: Cavities, Gum Disease, and Prosthetics

Cavities, periodontal disease (gum inflammation), impacted wisdom teeth, and poor prosthetic maintenance trap food and bacteria, leading to persistent odor.
Solution: Visit a dentist for exams to treat cavities, perform scaling/root planing for gum disease, or adjust prosthetics. Daily thorough brushing and flossing prevent progression; early intervention halts odor.
3) Tongue Coating and Poor Tongue Hygiene
The tongue’s surface harbors bacteria and debris (white coating or ‘setae’), contributing significantly to VSCs as it’s often overlooked.
Solution: Use a dedicated tongue scraper or soft brush daily after toothbrushing, starting from the back and moving forward gently to avoid irritation. This removes buildup more effectively than brushing alone.
4) Dry Mouth (Xerostomia)
Saliva naturally cleanses the mouth and neutralizes bacteria; reduced flow from mouth breathing, stress, medications (e.g., antihistamines, antidepressants), aging, or habits like smoking dries it out, worsening breath.
Solution: Drink 2 liters of water daily to stimulate saliva. Chew sugar-free gum to boost production. Avoid caffeine, alcohol, and tobacco. Humidify air at night and practice nasal breathing.
5) Diet and Lifestyle Factors
Foods like garlic, onions, spices, dairy, and proteins release sulfur compounds absorbed into the blood and lungs. Smoking, alcohol, coffee, irregular meals, and high-protein/low-carb diets exacerbate issues by promoting bacteria or dryness.
Solution: Limit odor-causing foods (garlic, onions, dairy); opt for fibrous vegetables, fruits, greens, and seaweeds rich in calcium/potassium to neutralize acids and clean teeth. Eat regular meals, starting with breakfast. Quit smoking and reduce coffee/alcohol.
6) Non-Oral Causes: Tonsils, Sinuses, and Systemic Issues

Though less common (10-20%), tonsil stones (debris in crypts), sinusitis, GERD, or diseases like diabetes, liver/kidney issues produce odors via post-nasal drip, reflux, or metabolic changes.
Solution: Gargle with saltwater for tonsils; see ENT for sinus/tonsil issues or gastroenterologist for reflux. Manage systemic conditions with physicians. Comprehensive evaluation by dentist, ENT, or internist if oral fixes fail.
How to Apply This in Practice
Daily Checklist for Fresh Breath:
- Brush teeth thoroughly 2-3 times daily (all surfaces, 2+ minutes).
- Floss and use interdental brushes once daily.
- Scrape/clean tongue gently every morning/evening.
- Drink water frequently (aim for 2L/day); chew sugar-free gum if dry.
- Eat balanced meals with veggies/fruits; avoid triggers like garlic/onions.
- Avoid tobacco, excess alcohol/coffee.
- Schedule dental check-ups and scaling every 6 months.
Track progress over 2 weeks; combine habits for best results. Avoid overusing mouthwashes, as they can dry the mouth.
Risk Note
Persistent bad breath despite hygiene may signal underlying issues like gum disease, infections, or systemic diseases (e.g., diabetes, GI disorders). Consult a dentist or physician promptly; self-treatment alone may delay diagnosis. Not medical advice—seek professional evaluation.










